I recently had the honor of presenting at the University of Illinois College of Medicine Well-Being Wednesday series and I’d like to share my slides on my evolving work on Post-Burnout Growth.


































I recently had the honor of presenting at the University of Illinois College of Medicine Well-Being Wednesday series and I’d like to share my slides on my evolving work on Post-Burnout Growth.








































This is the powerpoint of a talk I gave on 1/17/25 on Telemental Health and Burnout through the UW/Haborview TeleBehavioral Health Training Series. Thanks to the team for inviting me.















https://www.theinvisiblegorilla.com/IGvideos.html











My friend Lucy Houghton and I have been working on this idea of post-burnout growth, analogous to the concept of posttraumatic growth. We published a preliminary essay in Closler October 18, 2022 called A New Paradigm for Growth.
Since then I have continued to elaborate this concept and wrote about it in my latest book, Caring for Self & Others: Transforming Burnout, Compassion Fatigue, and Soul Loss. I would like to offer some sections of the book on the topic of post-burnout growth as a new paradigm for growing through suffering – burnout, compassion fatigue, and soul loss.
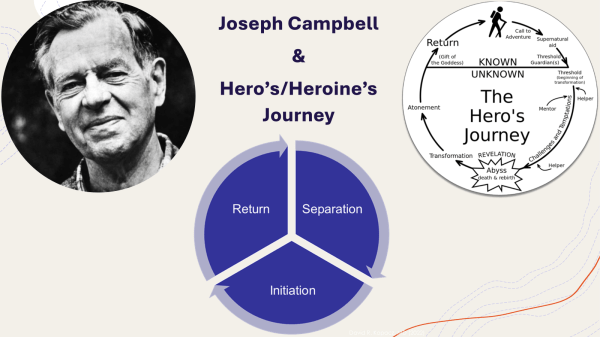
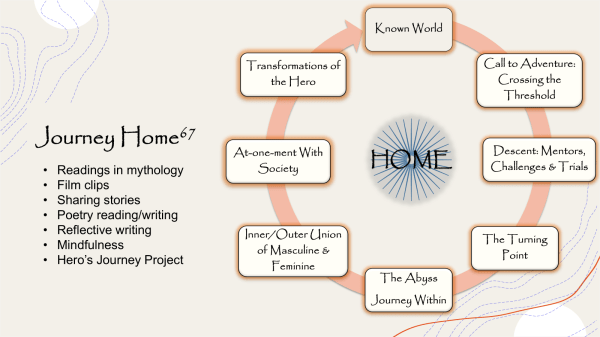
Initiation is a model of transformation that is ancient and is found in many Indigenous traditions as well as in the wisdom stories of many religions. In Becoming Medicine, Southern Ute elder Joseph Rael (Beautiful Painted Arrow) and I structured our book based on the three stages of initiation: separation, initiation, and return. While Joseph Campbell came to these stages through the study of stories and cultures, Joseph Rael has lived them through various initiation ceremonies in his education at Picuris Pueblo and the Southern Ute Reservation. Since 2014, Joseph and I have been working together, focusing on different ways that people can transform their own trauma and suffering by becoming healers―that is what it means to be becoming medicine: becoming a healer for yourself, others, and the world.
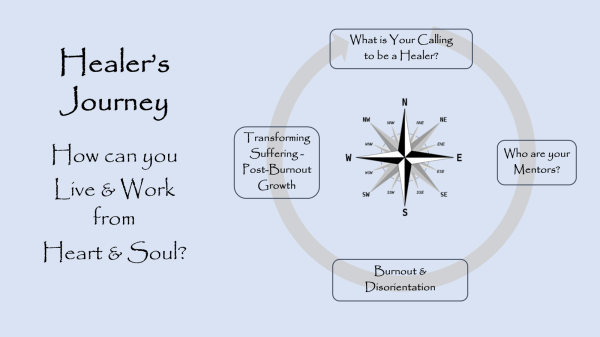
This kind of transformation is what Lucinda Houghton and I have been working on in regard to burnout. We have been calling this post-burnout growth, similar to posttraumatic growth―where suffering is used for personal and professional growth.[i] Posttraumatic growth has been described as: increased appreciation for life, more meaningful interpersonal relationships, increased sense of personal strength, changed priorities, and a richer existential and spiritual life.[ii] These are changes both in self as well as in relationships with others. We view post-burnout growth as not simple resilience of returning to who we were, but actually using suffering as a tool for growing beyond who we were into who we can become.
We can view burnout, compassion fatigue, and even soul loss as calls to initiation, just as Joseph Campbell described the call to adventure in the hero’s or heroine’s journey.[iii] The quest to reconnect with the soul is a kind of heroism that leads to healing. As storyteller Michael Meade tells us, “Life is change and the life of the soul is transformation.”[iv]
David Kopacz, Caring for Self & Others: Transforming Burnout, Compassion Fatigue, and Soul Loss. Palisade: Creative Courage Press, 2024, (pages 19-20)
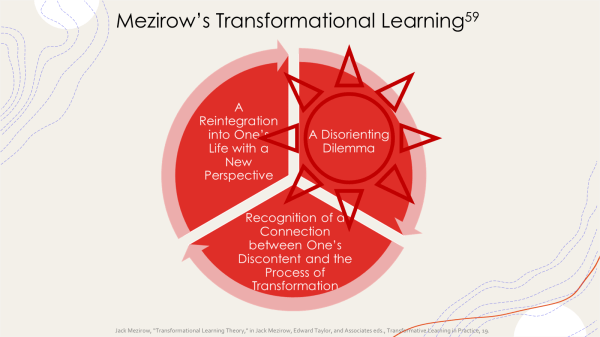
While burnout and compassion fatigue can feel like we have lost our souls, it is not so much our souls that are lost as we who are lost—we have lost touch with the innermost being of ourselves. As Joseph Rael teaches, Wah-Mah-Chi, Breath-Matter-Movement, holds back a place of goodness in each of our hearts, no matter what we have done and no matter what has been done to us. Burnout and compassion fatigue can be viewed as disorienting dilemmas that start the initiation of transformative learning―post-burnout growth! In this way, periodically losing touch with ourselves (our souls) is actually an ongoing invitation to enter into the healing space of transformational initiation. Our troubles, disorienting as they are, can be the call of transformation. “Thus,” writes Meade, “the troubles we find ourselves in are intended to wake us up to a greater sense of life and awaken the underlying soul, which knows better than us what our life is for.”[v] The loss of energy in burnout and compassion fatigue creates a space that offers us the opportunity to be guided by our inner knowing and inner wisdom of the soul. For, as Meade tells us, “when our energy drains from life’s outer projects, our attention is drawn inward, downward and back towards the original spark of our lives and the genuine project of our soul.”[vi]
Kopacz, Caring for Self & Others, pages (148-149)
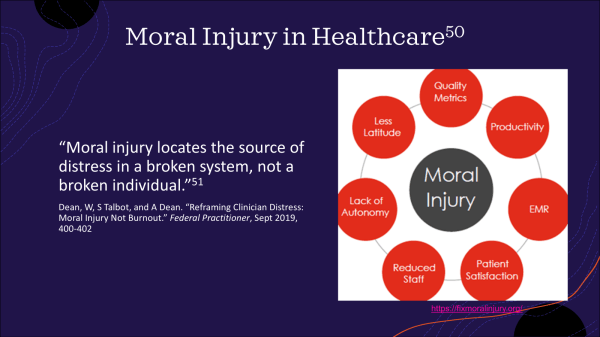
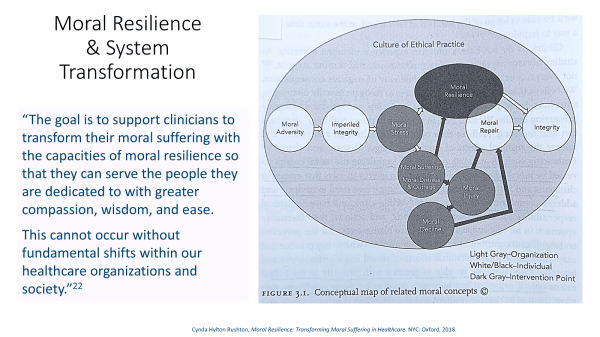
While resilience and self-care are part of the puzzle for recovering from burnout and soul loss, to only focus on these individual responsibilities runs the risk of blaming the victim. Are high rates of burnout actually due to the way our systems are designed? Swensen and Shanafelt think so, writing that the “current health care delivery system is perfectly designed to create high rates of professional burnout in physicians, nurses, advanced practice providers, and other health care professionals.”[vii] The problem, then, is not a lack of resilience within staff, but an institutional structure that does not support human flourishing. To address burnout and compassion fatigue, we have to go beyond individual resilience.[viii]
resilience (n.) “act of rebounding” … from Latin resiliens, present participle of resilire “to rebound, recoil,” from re- “back” … + salire ”to jump, leap”[ix]
While the ability to bounce back is important, we also need to transform, which means to grow beyond our previous limits. Transformation means we are not trying to be who we were, rather we are growing into the potential of who we can become. Many are questioning whether resilience is really the answer to the burnout pandemic, particularly within the field of posttraumatic growth. As Edith Shiro writes in The Unexpected Gift of Trauma: The Path to Posttraumatic Growth, “resilience doesn’t help us grow from adversity, it helps us cope with it, and further, “sometimes resilience actually hinders the possibility of achieving” posttraumatic growth.[x]
Richard Tedeschi and Lawrence Calhoun have been studying posttraumatic growth for years and they point out that “continuing personal distress and growth often coexist.”[xi] In this sense, the goal is not to be free of suffering, but to grow from it. This distinguishes a transformative growth paradigm from the prevention and recovery focus on work-readiness of the resilience paradigm. Rather than bouncing back to our previous level of adaptation, transformation helps us grow beyond it. Just as Chenrezig was not put back together with two arms and two eyes, we want to grow in the ability to see and touch suffering. Tedeschi and Calhoun describe posttraumatic growth as an experience where development “has surpassed what was present before the struggle with crises occurred,” and that this is not “simply a return to baseline―it is an experience of improvement that for some persons is deeply profound.” Posttraumatic growth “has a quality of transformation…unlike…resilience.”[xii]
Resilience and subjective well-being can be part of the approach to burnout, compassion fatigue, and soul loss, but only take us so far―they can restore previous functioning, but do not help us grow as healers or as human beings. Posttraumatic growth and post-burnout growth are transformation paradigms that take us beyond resilience, however we still need to look beyond the individual to the health care ecosystems we work in and the institutional variables that contribute to burnout, maintain it, and limit our focus to being the same productive work unit we were yesterday instead of supporting a transformational growth mindset. It is worth re-examining the costs of caring again, this time looking at the systemic and organizational issues, as we have been covering the personal and individual levels. We can look at the costs of caring from a different perspective after taking the journey of caring for self & others. Each cost of suffering can be seen as having a joyful counterpart: from burnout to post-burnout growth, from trauma to posttraumatic growth, from dehumanization to re-humanization, from demoralization to remoralization, from soul loss to soul recovery, and from suicide to finding meaning and purpose which leads to joy and flourishing. It is not easy work to dig ourselves out of the abyss of the costs of caring and to return, transformed, back into the health care world armed with our rejuvenated joys of caring.
Working with people is stressful and exposes us to direct and vicarious trauma. We can’t eliminate exposure to suffering from our work. But we can build in ways to grow in our capacity for caring―this doesn’t mean never suffering, but developing a greater capacity to work with suffering. In addition to individual approaches, we also need to go beyond resilience to create organizations that measure employee idealism and well-being as well as measuring productivity. As the late Alessandra Pigni, a former Doctors Without Borders psychologist, stated:
But is self-care enough to prevent burnout? Yes and no. There is self-care as in “a day at the spa,” recreational self-care, and there is self-care as “care of the self,” a deeper kind of attention to ourselves, the sort that asks questions like, “What am I doing in this group/organization/community? Do I still belong here?” We call this transformational self-care.[xii]
Alessandra Pigni, The Idealist’s Survival Kit: 75 Simple Ways to Avoid Burnout
Transformational “care of the self” challenges us to look not just at ourselves as individuals, but how we fit in the larger institution. If an institution is not supporting our humanity and for whatever reason we are not able or in a position to transform the institution, that may mean we care for ourselves by changing jobs. If transformation is possible, then we roll up our sleeves and contribute to the challenging work of transforming systems and institutions.
Kopacz, Caring for Self & Others, pages (209-212)

References
[i] David Kopacz and Lucinda Houghton, “A New Paradigm for Growth,” CLOSLER, October 18, 2022, https://closler.org/lifelong-learning-in-clinical-excellence/a-new-paradigm-for-growth.
[ii] Richard G. Tedeschi and Lawrence G. Calhoun, “TARGET ARTICLE: ‘Posttraumatic Growth: Conceptual Foundations and Empirical Evidence,’” Psychological Inquiry 15, no. 1 (2004): 1–18, https://doi.org/10.1207/s15327965pli1501_01.
[iii] Campbell focused primarily on the masculine hero’s journey. Other authors have further developed the heroine’s journey, for instance Maureen Murdock’s The Heroine’s Journey and Marina Tatar’s The Heroine with 1001 Faces.
[iv] Michael Meade, Awakening the Soul: A Deep Response to a Troubled World (Vashon, WA: Greenfire Press, 2018), 73.
[v] Ibid., 120.
[vi] Ibid., 128.
[vii] Swensen and Shanafelt, Strategies to Reduce Burnout, 37.
[viii] Kopacz, “Beyond Resilience.”
[ix] Online Etymology Dictionary, s.v. “resilience,” accessed April 7, 2022, https://www.etymonline.com/word/resilience.
[x] Edith Shiro, The Unexpected Gift of Trauma: The Path to Posttraumatic Growth (New York: Harvest, 2023), 60–61.
[xi] Tedeschi and Calhoun, “Posttraumatic Growth,” 2.
[xii] Ibid., 4.
[xiii] Alessandra Pigni, The Idealist’s Survival Kit: 75 Simple Ways to Avoid Burnout (Berkeley, CA: Parallax Press, 2016), 55.
I’ve been thinking about how we need to build a community of practitioners discussing the problems of burnout, compassion fatigue, and soul loss. Isolation and loneliness contribute to burnout, and social connection is an antidote to burnout. To this end, we are creating the Becoming A True Human podcast. Who is “we”? Well, for now, it is me and my good friend Chris Smith – therapist, meditation teacher, Whole Health educator, storyteller, author (Be a Good Story), founder of the Academy for Mindfulness consulting, and all-around wise guy (and I mean that in multiple senses of the phrase).
The audio of the episode 1, Lost, is at the bottom of this post.


What is burnout? Just what exactly is it that burns out? How can whatever is burned out be re-ignited?
What is compassion fatigue? How does compassion wear out? Should it really be called empathy fatigue? Is the problem that there is too much compassion going out? Or not enough coming in? Or could it be that institutional structures and protocols make us busy with so many things that there is little time left in the clinical encounter for caring?
What is soul loss? Could we think of the soul being the “thing” that burns out? Not necessarily in a religious or metaphysical sense – although it could be if that fits your belief system – but in a metaphorical and psychological sense. If in burnout we lose connection with our souls, how can we reconnect and either go on a quest to find our lost souls, or create a welcoming environment in our bodies and lives so that our souls can return and flourish?
I address these questions in my book, Caring for Self & Others: Transforming Burnout, Compassion Fatigue, and Soul Loss, but we need to have further discussions around these topics as I feel strongly that we need a kind of ongoing practice, a yoga of burnout, in which we continually work in our own practices as well as in building communities of caring to support each other with this human, all too human dilemma.
Based on the topics we discussed in the first episode we titled this episode “Lost,” even before we realized that we somehow lost video of me and only recorded video for Chris! In this episode we explore topics of burnout as an initiation into becoming a wounded healer, soul loss, yoga for the health of healers, and we end with a meditation exercise and a poem, “Lost” by David Wagoner.
We don’t really know what we are doing with the technology aspect.
Let me tell you a story that illustrates the problem.
My high school friend Jack and I drove across the country after college. We were into the beat poets and writers, reading Kerouac’s On the Road, and envisoned a trip full of excitement and philosophical observations. We had a microcassette recorder and would talk into as we were driving, having many deep discussions and creating a record of what we saw.
Somewhere around South Dakota (having left from Chicago area) I noticed that the wheels of the recorder weren’t moving when we were recording. It was then that I noticed that there was a pause switch that was clicked on and prevented any recordings from being made! All of our bits, routines, observations, and experiences were lost! We were a bit crestfallen and we made half-hearted attempt to resume recording, but something had been lost – the energy, the enthusiasm. I think we eventually gave up on it. Maybe you could say we burned out on the idea after investing so much energy and enthusiasm and not having anything to show for it.
From a mindfulness perspective, there is surely some kind of lesson here – about not being attached to goals or outcomes, about being in the present moment versus memorializing experience, and maybe even that the organizing ego is an illusionary construct for creating a reduced and more manageable limited reality (if you want to take it that far!).
Well…I remembered this story after Chris Smith and I had just had our wide-ranging and enthusiastic discussion as we recoreded it on Zoom, only to realize that I had messed up the settings and we only had Chris’ video and both our audio. Well, crestfallen again! Urgh, technology failure again!
So, I think I have figured out how to share the audio of our video podcast, rather than have video of just Chris and my disembodied voice. Titling this episode, “Lost,” was prescient as we lost the video. Chris also spoke of his caring for self routine and how he purposefully skips some days so as not to get caught up in perfectionism, performance, and productivity. We’ll consider the lost video as a sacrifice to the Divine or the Cosmos, a giveaway, in addition to it being a bumbling failure of technology.
So, welcome to the first episode of the Becoming A True Human podcast – Lost – it highlights the vulnerability and imperfection of being human, that we are all a work in progress and that our work is a yoga practice – yoking mind, emotions, body, soul. The practice of Becoming A True Human is an ongoing practice, we can only do it in the present moment and the next moment we are again lost, at sea, trying to figure it out and Keep It All Together (KIAT). We will attempt to have the next episode as video and hope to post it on the Becoming a True Human YouTube site.


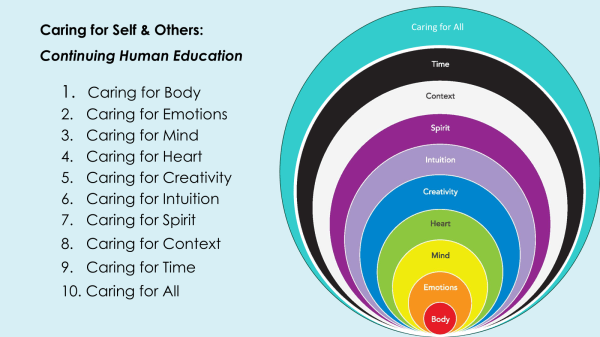
I have been working on this book for ten years – the longest of any book I’ve written. In many ways it is a follow-up of Re-humanizing Medicine (2014) and yet it also is strongly influenced by my work over the past 10 years with Joseph Rael (Beautiful Painted Arrow). It brings together my work on physician and staff wellness in presentations and workshops, from my work Whole Health at the VA, and my work with The Doctor as a Humanist. Re-humanizing Medicine used a 9-dimensional model of the components of being fully human: body, emotions, mind, heart, creativity, intuition, spirituality, context, and time. In Caring for Self & Others, I’ve added the dimension of Becoming Caring: Caring for All, a kind of holistic leadership for self & others. Within each of the ten different dimensions of being fully human I have developed three different domains that end in an -ing (in honor of Joseph Rael’s emphasis on verb-ing in our conversations). I’ll now give a brief review of the journey of how this book has come into being.

After publishing Re-humanizing Medicine, I realized I needed to develop a set of practices to operationalize what I called the counter-curriculum. The counter-curriculum was a humanizing curriculum, a caring for self curriculum, which focused on how we do things, not just what we do in clinical settings. If our medical education and continuing medical education (CME) trains us to be good clinicians, the counter-curriculum trains us to be good human beings – thus I came to call this Continuing Human Education (CHE). In the age-old balance of being healers and technicians, I recognized that we have really given the education of ourselves as healers short shrift, and have almost exclusively focused on becoming technicians at the expense of our humanity. The loss of our role as healers and the loss of our human presence in medicine leads not only to impoverished clinical care (with patients feeling like they are being processed by protocols rather than cared for by human beings), but it also cut us off from the rejuvenating nature of the healing relationship which nourishes our own humanity as well as the humanity of our patients and clients. I realized that to care for others we must first care for ourselves and that in caring for ourselves we were developing the skills and aptitudes necessary to care for others.
In 2015 I was developing the idea of “Becoming a Whole Person to Treat a Whole Person,” which I presented in various forms at the Australasian Doctors’ Health Conference, and conferences of the Alliance of International Aromatherapists, and the Australasian Integrative Medicine Association.
In 2016, Joseph Rael and I published Walking the Medicine Wheel: Healing Trauma & PTSD. That year I deveoped presenations on Healing Circles, Pathways to Healing Moral Injury, and comparing the Medicine Wheel and the Hero’s Journey as pathways of initiation and healing – with presentations at the Mayo Clinic Humanities & Medicine Symposium, and various local settings. I developed a half-day workshop called “Caring for Self: Well-Being in the Workplace” that I gave for HopeWest hospice staff in Grand Junction, CO.
In 2017 I first started using the title of “Caring for Self & Others” in presentations, for instance at Western Sydney University in Australia. I continued developing ideas around Healing Circles and the Hero’s Journey, with presentations at the Australasian Doctors’ Health Conference and the University of the South Pacific in Fiji.
One of the dimensions of being fully human from Re-humanizing Medicine was spirituality and I had a sub-section on mysticism and medicine. My work with Joseph Rael, which has resulted in the publication of four books thus far, has allowed an in-depth exploration of the role of spirituality in healing. Our 2020 publication of Becoming Medicine: Pathways of Initiation into a Living Spirituality was a blending of Joseph Rael’s teachings within a framework of initiation, a review of healing through the lives and writings of visionaries, mystics, and shamans, and a survey of the perrenial philosophy of timeless healing wisdom. My subsequent training as an iRest certified teacher (a Western adaptation of yoga nidra from Kashmiri Shaivism by psychologist Richard Miller) and as a certified yoga teacher (CYT 200), has allowed me to study and explore nondualistic states – which I feel are foundational to breaking down the barriers between self and other – a kind of nondual medicine, as I call it in Caring for Self & Others.
As I have been working with burnout for myself and in staff and clinicians, I started to realize that there were many terms for health care worker suffering, not just burnout, but compassion fatigue, secondary and vicarious traumatization, PTSD, demoralization, moral injury, and even suicide could be an outcome of the burden of caring for others. I have come to use the term the costs of caring to encompass all these different dimensions of staff and clinician suffering. My good friend Greg Serpa and I published a chapter on “Clinician Resilience” in the Integrative Medicine, 5th edition textbook and I started to bring together a number of ideas I had been working on around burnout, moral injury, and the costs of caring, and even the idea of soul loss.
Soul loss is often considered one of the causes of illness in shamanic and indigenous traditions, such as in the work of Joseph Rael. It also has a resonance with the Western traditions that psychiatry and psychotherapy grow out of. The etymology of the word “psychiatry” comes from the Greek words psyche + iatros, soul healer. The Swiss psychiatrist, Carl Jung, frequently wrote of the psyche and also of the soul in his work as a healer and psychotherapist. The more recent, modern tradition of neglects the idea of the a vital essence of a person – yet there is a practical utility in addressing burnout as “soul loss.” In doctors and health care workers, as well as in teachers, and business, burnout is such a serious issue. We talk about burnout, but what is it that burns out? The soul is one answer – not necessarily in a metaphysical or religious sense, although it could be understood that way, but in a metaphorical and evocative way of describing what burnout and compassion fatigue feel like – that one has lost some core aspect of one’s being – a loss of soul. I gave presentations on burnout and soul loss at the Doctor as a Humanist’s on-line international conference, New Realities in the Times of COVID-19 (2020), University of Washington Psychiatry Grand Rounds (2021), and Seattle University’s Giving Voice to Experience Conference (2022).
A key idea in Caring for Self & Others is that suffering can be transformed – this is what healing is all about and this is the primary skill that a healer has, how to transform suffering. Our work as healers, doctors, technicians involves exposure to suffering, therefore we cannot eliminate suffering from our work as the very definition of our work is to engage with suffering. We can minimize the amount of collateral suffering that we experience from working in systems that do not support the full human being of clinicians and staff – that is the moral injury piece that we need to address. However, I think that burnout is inevitable when we are people who work with people, particularly people who work with suffering people. In my conversations during the pandemic, Lucy Houghton and I have been developing the idea of post-burnout growth, which is analogous to post-traumatic growth, in which we use suffering as a stimulus to personal and professional growth. Post-burnout growth captures the idea that burnout is not to be feared, but rather respected as a predictable occupational hazard – just like a firefighter working with fires is sooner or later going to get burned.

The story of Chenrezig as a wounded healer captures this idea of post-burnout growth perfectly. Chenrezig vowed to alleviate all suffering in the world – which is not dissimilar to our own vows, spoken or unspoken, to heal others. If he was not successful in this vow, he pledged that he would shatter into a thousand pieces – a state akin to burnout, compassion fatigue, and soul loss, where we feel injured as a result of our caring. This is, in fact, is what happened – Chenrezig worked diligently, healing many, yet there was still more suffering than he could address and he shattered into a thousand pieces. This is where the story ends for so many health care workers and educators who become embittered, cynical, and maybe even leave their profession. But in the story of Chenrezig, there is a ritual elder, Avalokiteśvara, who sees Chenrezig’s suffering from addressing others suffering. Avalokiteśvara puts Chenrezig back together – not simply as he was before (this is my problem with the way resilience is often used in health care – as a way of going back to the past, or avoiding suffering), but rather as having a thousand eyes to better see suffering and a thousand arms to better touch suffering. Chenrezig becomes more capable of seeing and touching suffering – through post-burnout growth.
This book, Caring for Self & Others: Transforming Burnout, Compassion Fatigue, and Soul Loss, has grown over the last ten years and I am grateful to all the above mentioned organizations. The book and I have also been shaped by numerous conversations with friends and colleagues and I would particularly like to thank Laura Merrit, Shelly Francis (Creative Courage Press), Joseph Rael (Beautiful Painted Arrow), Steve Hunt, Jonathan McFarland, Usha Akella (The POV), J. Greg Serpa, Tulika Singh, Chris Smith, Lucy Houghton, Transformational Arts Network and their Power of Words conference, Gretchen Miller (and the editorial staff at the CLOSLER blog), and so, so, so many others. There truly is no self without others.


We’ve gotten some really nice endorsements for the upcoming release of Caring for Self & Others: Transforming Burnout, Compassion Fatigue, and Soul Loss – which will be released on June 25th and is currently available for pre-order through Amazon. I’ll share some of the comments below:
Jean Watson, PhD, RN, AHN-BC, FAAN, LL (AAN), Founder Watson Caring Science Institute, Distinguished Prof/Dean Emerita University of Colorado Denver, College of Nursing
Dr. Dina Glouberman, author of The Joy of Burnout: How the end of the world can be a new beginning
Mukta Panda, MD, author of Resilient Threads: Weaving Joy and Meaning into Well-Being and co-author of The Oath to Self-Care and Well-Being
Marianela Medrano, PhD, What a Word is Worth podcast, and author of Rooting, Diosas de la yuca, and other titles
Shaun McNiff, PhD, author of Art as Medicine, Art Heals, Integrating the Arts in Therapy, Trust the Process: An Artist’s Guide to Letting Go, Imagination in Action: Secrets for Unleashing Creative Expression, and other books. Lesley University, Cambridge, MA, 2021 to date: University Professor Emeritus
Lucia Thornton, ThD, MSN, RN, Past President, American Holistic Nurses Association, Past President, Academy of Integrative Health and Medicine, and author of Whole Person Caring: An Interprofessional Model for Healing and Wellness
Kate King, MA, LPC, ATR-BC, author of The Radiant Life Project
John (Jack) Miller, Professor at the University of Toronto and author of Education and the Soul, Love and Compassion: Exploring Their Role in Education, and A Holistic Educator’s Journey: Seeking Wholeness in America, Canada, Japan and AsiaThe Holistic Curriculum
Stephen Cope, Scholar Emeritus, Kripalu Center, bestselling author of The Great Work of Your Life, The Wisdom of Yoga: A Seeker’s Guide to Extraordinary Living, and The Dharma in Difficult Times: Finding Your Calling in Times of Loss, Change, Struggle, and Doubt
Jonathan McFarland, MA, President and Founder of The Doctor as a Humanist and co-editor of Health Humanities for Quality of Care in Times of COVID -19, Associate Professor, Universidad Autónoma de Madrid

Caring for Self & Others: Transforming Burnout, Compassion Fatigue, and Soul Loss will be published by Creative Courage Press – thanks to Shelly Francis for all the support in the publication process!
I will be giving a keynote presentation at the 13th annual Giving Voice to Experience conference, whose theme is “Maintaining a Soulful Approach to Psychological Research and Practice: Swimming Upstream in a Technological Society.”
My talk on “Burnout: Soul Loss & Soul Recovery” seems even more relevant now than it did when the conference was originally planned for March of 2020 – at that time the pandemic was just evolving and we didn’t know one day to the next whether we would be gathering or not. I was already, at that time, beginning to look at the similarities between burnout in health care and the ancient concept of soul loss. After all, what is it that stops burning in burnout? What is it that we lose when we feel we are just pushing ourselves through the motions at work? Where have our hearts gone? Where have our souls gone? Now, after two years of pandemic life and social distancing, as well as the larger social injustice issues and division in the USA and war and conflict in the world, it seems even more vital than ever that we re-connect to that which makes us fully human.
For a number of years, Seattle University used to host the Search for Meaning Book Fesitval that I attended regularly. It saddens me that SU is no longer running that program since 2017, but I am honored to speak there and be part of the tradition of inquiry into life’s meaning and greater purpose. Here is the abstract for the talk:
Burnout and compassion fatigue are becoming the norm in healthcare after two years of a pandemic. The World Health Organization recognizes burnout as an “occupational phenomenon,” with feelings of energy depletion; increased mental distance from one’s job, negativism, and cynicism; and reduced professional efficacy. While many perspectives on burnout focus on prevention through stress management techniques, we can look at burnout as “soul loss” which can then become the beginning of a transformational healer’s journey. A transformational perspective shifts our focus to the care of the soul and on how to recover soul once it is lost – this is a valuable skill for us as healers to use in our own lives as well as in our therapeutic work with clients.
David Kopacz is a psychiatrist in Primary Care Mental Health at Seattle VA and a National Education Champion with the VA Office of Patient Centered Care & Cultural Transformation. He is an Assistant Professor at University of Washington and is certified through the American Boards of: Psychiatry & Neurology; Integrative & Holistic Medicine; and Integrative Medicine. David is a graduate of University of Illinois, undergraduate in Urbana-Champaign and medical school and psychiatric residency in Chicago. He has practiced in the US and New Zealand. His publications include: Re-humanizing Medicine: A Holistic Framework for Transforming Your Self, Your Practice, and the Culture of Medicine; Caring for Self & Others: Transforming Burnout, Compassion Fatigue, and Soul Loss (in press); and with Joseph Rael (Beautiful Painted Arrow) Walking the Medicine Wheel: Healing Trauma & PTSD; Becoming Medicine: Pathways of Initiation into a Living Spirituality; Becoming Who You Are: Beautiful Painted Arrow’s Life & Lessons for Children Ages 10-100.
Here is the link to the conference for registration and a flier for the conference. 6 CEUs are available for the one day conference. For further information about the conference, please contact Professor Steen Halling: shalling@seattleu.edu
How are you doing…really? New post on CLOSLER: Bringing Us Closer to Osler

This is a reflection piece on the challenge of answering this simple question, asked so many times a day, “How are you doing?” While this is usually asked in passing, the true answer to this question is increasingly complex for health care workers as the pandemic wears on.
You can read the essay, here, and some past essays published on CLOSLER, here. The piece features a detail of my painting, “Planting the Seed of the Heart,” which was published in Walking the Medicine Wheel: Healing Trauma & PTSD.
Thanks again, CLOSLER, for all that you do for person-centered care & provider well-being!

I will be presenting “Burnout: Soul Loss & Recovery in Health Care” at this free virtual international symposium sponsored by The Doctor as Humanist, McGraw Hill, Sechenov University, and Universidad Anáhuac México.



This is a talk that I prepared for Seattle University’s 13th Annual Giving Voice to Experience Conference, “Maintaining a Soulful Approach to Psychological Research and Practice: Swimming Upstream in a Technological Society.” It was to have been on 3/7/20, but it was cancelled as Washington state began shutting down due to the COVID-19 Coronavirus. I thought that I could at least get it out there through my blog. The conference will likely be rescheduled in the future, but until then, I’ll release these slides out into the world. We need to come up with creative ways of sharing information and creating community in these times when we cannot gather together. As my friend Suzanne Richman recently said, “Technology is the new architecture of how people gather.” She says the idea is not her’s, she was paraphrasing a talk by a Rabbi she heard on Martin Buber.











































