As we enter into a new phase of the pandemic, I worry about myself and my colleagues in health care – how will we come out of this? How will health care change? When will we feel like we have recovered from the constant changes and worries about our personal and collective health?
I’ve been working for a while on a workbook adaptation of Re-humanizing Medicine. I’ve been seeing if I can get this published or figure out a way to get it out to the larger world as a resource for caring for ourselves & others. I’m not sure exactly what form this will take, but in the meantime, I thought it might be worth revisiting some of the concepts and topics of Re-humanizing Medicine: A Holistic Framework for Transforming Yourself, Your Practice, and the Culture of Medicine that I published in 2014.
I’d like to give a few quotes from the book and put them out into the world as a small offering to address the suffering, burnout, compassion fatigue, soul loss, and moral injury of health care colleagues. The experience of dehumanization is all to prevalent in contemporary medicine and the need for re-humanization is just as needed as ever! Here is the introduction to the book:
Introduction
Only connect! … Live in fragments no longer.
E.M. Forster1
The great error of our day in the treatment of the human body is that physicians first separate the soul from the body.
Plato2
Dehumanization in Contemporary Medicine
This book takes on the task of re-humanizing medicine. We start by recognizing that there is a problem with how medicine is currently practiced: it dehumanizes staff and clients, creating dissatisfaction, suffering, poor performance and medical errors. Dehumanization is an iatrogenic effect of the dominant paradigms in contemporary medicine – the economic/business model and the reductionist and materialistic approach of biomedicine. In the day-to-day practice of medicine, doctors are expected to see more patients in less time and to efficiently reduce people to symptoms, diagnostic codes, prescriptions, procedures and billing codes. This leaves little time or space for people – physician or patient.
Future doctors are attracted to medicine for idealistic and humanitarian reasons, but through training they often lose this idealism.3,4 How can we preserve idealism and humanitarianism in medicine? Practicing physicians have high rates of burnout and job dissatisfaction. How can we reinvigorate the practice of medicine and make it sustainable?
A Counter-Curriculum of Re-Humanization
In medical school, I realized that I had to engage in a parallel education process in addition to the standard scientific curriculum. We could even call this a ‘counter-curriculum’, focusing on re-humanization. At times I found teachers, mentors, and fellow students who practiced this counter-curriculum, but often I had to seek it out on my own in order to balance my education. This book is about that counter-curriculum of re-humanization. Science and evidence-based interventions are one paradigm of medicine, but as human beings working with human beings, we must have a human framework as well as a scientific one.
As a medical student, the first research project I worked on was with Deb Klamen and Linda Grossman at the University of Illinois at Chicago. Our study examined symptoms of Posttraumatic Stress Disorder (PTSD) in relation to medical training and found that 13% of trainees in the study reported sufficient symptoms (relating to their internship year) to potentially qualify for a PTSD diagnosis.5 The findings provide evidence supporting the need to change postgraduate medical education to reduce stress and to enhance the well-being of trainees. I went on to work with Linda and Deb on three other papers that examined medical students’ beliefs and their attitudes toward the controversial issues of homosexuality, abortion, and AIDS.6,7,8 These papers examined how medical student beliefs can shape attitudes that adversely impact medical care. The studies also allude to the fact that people are not purely rational beings, and beliefs, fears and stigma can undermine scientific reasoning or professional ethics. Even my student research experience was concerned with the counter-curriculum of exposing dehumanization and seeking re-humanization.
To re-humanize medicine, the people who work in medicine must be well-rounded, well-developed human beings, as well as safe and effective technicians. A great deal of time, energy, and money is spent in making sure that physicians are good technicians, but are they good human beings? Being a good technician (objective, detached, unaffected by emotion, protocol-driven) can actually interfere with being a good human being. Clinicians should not stop being technicians or scientists, but they have a responsibility to attend to their own humanity, as well as that of the client. The counter-curriculum provides a holistic framework for being a human being, for working with human beings, and for creating systems that deliver care by human beings to human beings.
A Holistic Framework for Medicine
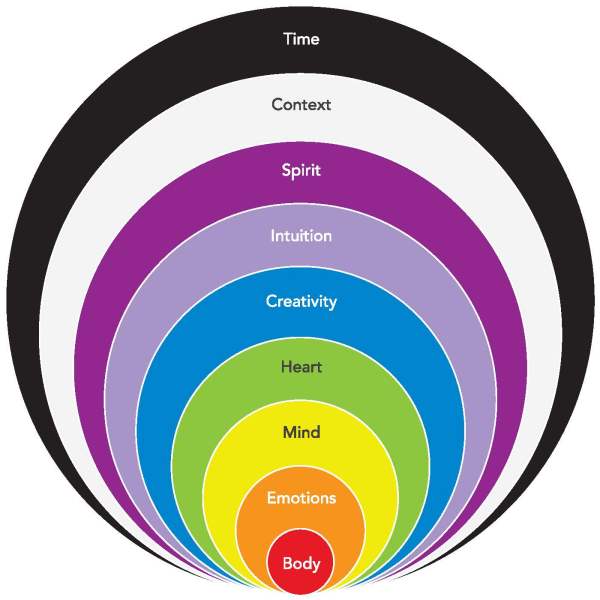
A holistic framework is founded on multiple interacting and mutually influencing sub-systems. Scientific medicine and the objective, observable body make up just one dimension of human health. Sometimes the physical dimension is primary, for instance in physical trauma and surgery. Sometimes other human dimensions are more important. Emotion, mind, love, self-expression, intuition, spirituality, context and time all play a role in health and illness.
A holistic framework is a paradigm for understanding and interacting with human beings. It is a human systems approach and a way of being in the world. Holistic medicine is a philosophy, or a paradigm for understanding what it is to be human, to suffer, to be ill, to be healthy; what it is to change, grow and live. It helps us understand how disconnection can lead to suffering and how connection can lead to healing. Holistic medicine is not defined by using an herb instead of a medication, or by any specific technique or intervention. Being a good technician (whether biomedical or ‘natural’) is part of being a good physician, but being a good physician is more than just being a good technician.
It is hard work to maintain a complex identity that includes being a technician and a human being, but that is what being a medical professional involves: balancing different roles for the purpose of alleviating suffering and treating disease. Re-humanization reconnects the art and science of medicine, the heart and the mind. A holistic framework encourages integration.
When you start to connect in a different way, you change the health care delivery system in which you work. What starts as personal dissatisfaction can become personal transformation, which changes systems. Institutions will always drift toward promoting their own interests over human interests. It is the responsibility of health professionals to ensure that they stay human, help their clients stay human, and ensure that health care delivery systems promote humanization rather than dehumanization.
Intended Audience and Purpose of the Book
I wrote this book for people who are looking for different ways of thinking about and practicing medicine. Dehumanization in medicine occurs throughout the world, particularly as business models replace humanitarian models of care. Many of the examples in the book are specific to the United States or New Zealand, drawing on my experience of practicing medicine in various settings in both countries; but whether dehumanization results from the profit motive of an insurance company (as in the US) or the bureaucratic processes of a national health system (as in New Zealand), the effect is the same. Re-humanizing medicine is a universal need.
This book is written specifically for clinicians, doctors, and physicians,9 who face daily humanitarian10 challenges in their roles, but is of interest to any health care professional or administrator. There are many fields where the application of a trained technique interferes with human connection, so teachers, trainers, educators and business people will find it relevant too. Of course, so will anyone interested in being a whole human being!
Since holistic medicine is a philosophy and a mode of being, I do not list diagnoses and alternative treatments. There are already a number of excellent books that review various complementary, alternative, and integrative medical techniques. The foundation of a holistic medical practice is you, not the services and techniques that you offer. Therefore, this is a book for people who are willing to change at a personal level in order to be better doctors and clinicians.
Contemporary medicine and holistic medicine are not inherently in conflict. My hope is that by defining holistic medicine as a paradigm, rather than as a specific technique, its benefits can be integrated with those of contemporary medicine. My primary argument is that the human elements of medicine need to be valued so that technical interventions occur within a human context.
Holistic Medicine, Re-humanization and the Quality Revolution in Health Care – A Convergence?
There is a worldwide trend in health care that, interestingly, overlaps with the philosophy of holistic medicine. This trend is a focus on quality, efficacy and safety, stimulated by the continual increase in the cost of health care. Experts are calling for a ‘revolution in health care delivery,’11 and ‘system-wide change.’12
Many of the suggestions involve cost-cutting and standardization of treatment. The ‘Quality Revolution’ also raises issues related to re-humanization, such as putting the patient at the center of treatment, making decisions collaboratively, and establishing a ‘continuous healing relationship.’13 These are the strengths of a holistic framework – not only is it patient-centered, but it includes the concept of healing in addition to treatment, and it often encourages low-cost, low-risk lifestyle changes and preventative medicine. It may be that it is time for a Compassion Revolution and a Quality Revolution to join forces in order to make medicine more affordable, safe and effective, as well as more compassionate, caring and human.
Structure of the Book
The book is divided into five major parts. The first discusses the underlying paradigms of the biomedical and economic models of contemporary medicine and how these models have side effects of dehumanization. This critique does not mean that there is no benefit in the contemporary paradigm; rather it is an examination of the strengths and weaknesses of the underlying paradigms of the current system. The second part describes the paradigm of holistic medicine as a way of understanding the whole person. The third part is a ‘self-help’ section that outlines how you, as a clinician, can develop a more holistic and deeper sense of your own humanity. The fourth part is a ‘how-to’ component that describes how to create a holistic practice in any setting and how to re-humanize your practice. The last part describes the benefits of a holistic paradigm for re-humanizing the culture of medicine.





























![logo-cr[1]](https://beingfullyhuman.com/wp-content/uploads/2015/01/logo-cr1.png)
![jhp53db8b682bd57[1]](https://beingfullyhuman.com/wp-content/uploads/2014/08/jhp53db8b682bd571.jpg?w=195)
![Kopacz-read[1]](https://beingfullyhuman.com/wp-content/uploads/2015/01/kopacz-read1.jpg?w=300)
![Kopacz-robot_1[1]](https://beingfullyhuman.com/wp-content/uploads/2015/01/kopacz-robot_11.jpg?w=300)